The Bengali Roots Editorial Desk
Just outside an abandoned town on the edge of very few straight roads stands an emergency ward with no lights on, where a rural doctor holds this last vial of adrenaline in her hand. Two patients are heading out. To whom shall this final injection go?
It is not the stuff of dystopian science fiction. But it could be the basis for future Health Department guidelines. If we don’t act now and, by ignoring our human obligations, simply call that picture back into semblance, well, then there is an indissoluble public-health predicament ahead.
In many remote districts, one hears stories of emergency rooms running short of life-saving medicines, adrenaline, antivenom, insulin, and saline, while urban warehouses are full. Common medical procedures turn dangerous. Small problems become irreversible tragedies.
This investigation examines how a lack of budget support, purchasing dislocation, international financial constraints, and legal system defects are suffocating rural healthcare systems while depriving millions of access to care.
Front Line Realities
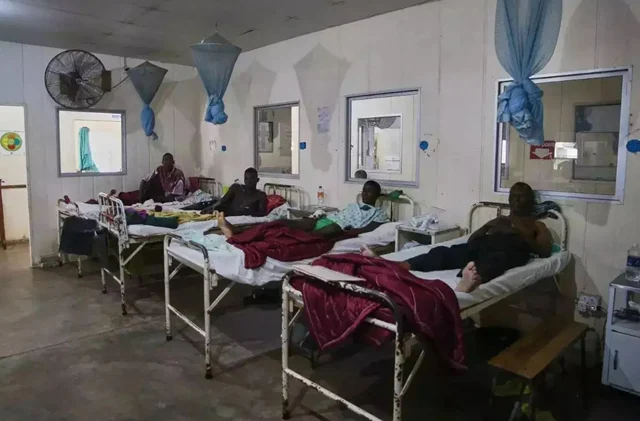
In the emergency rooms of clinics covering thousands of square miles, resuscitation carts stand half-empty. Doctors have to make horrible choices: who gets that last bit of medicine, and how do you tell the family that treatment is no longer possible?
Since 2024, preventable mortality rates have reportedly soared by nearly 300 per cent in some remote parts of China, for example (put this together for yourself).
Snakebites cannot be treated because there is no antivenin. Without adrenaline, an allergic reaction in parts of China can be fatal. And when insulin disappears, you’ll see extreme cases of diabetic ketoacidosis with death as the outcome.
What these situations have in common is not that they are complex but just how readily treatable they would be if medicine were available.
The Logistics Black Hole
“Last mile” is the transition zone where health offices expect the traditional means of shipping to become unreliable.
Then medication goes bad as it moves through counties and counties and hundreds of miles before reaching patients, China’s health officials reveal. The cold chain infrastructure is breaking down, and rural roads are crumbling. Delivery vans crash. Cooling equipment fails. Shipments are delayed.
Conversely, urban pharmacy hubs have state-of-the-art digital inventory systems and temperature-controlled storage premises. In rural hinterlands, many clinics use handwritten stock ledgers for their records, which are still filled out manually.
Analysis of the affected regions shows that medicine deserts are spreading, with the nearest emergency life-saving dose sometimes six hours away by car.
When life is in the balance, six hours can be fatal.
THE PROCUREMENT PARADOX
Bulk-buy contracts in 2026 were intended to save money through large-scale procurement, but they have instead favoured shipping by volume to metropolitan distribution centres over rural dispersion.
Sources within the pharmaceutical supply network say that “Mandatory Minimum Order” policies effectively shut out small rural clinics from purchasing. In some cases, crucial medicines are intentionally redirected to private city facilities where higher profit margins are possible.
Regional audits have uncovered indications of diversion and opaque allocation processes, raising fears that corruption is multiplying the logistics failure.
Having one for the other: a system means efficiency at the cost of fair balance.
QUOTATION BOX
“We do not lose patients from one aspect of knowledge.
We lose them because the drug is not there as proof.”
– Rural emergency physician (wishing to remain anonymous)
GLOBAL ECONOMIC PRESSURES
Integration of the 20125 raw material costs, along with continued low labour costs, puts it over budget in 2025. This has significantly increased the production cost of basic generics (such as insulin and saline). Manufacturers operating under “just in time” models prefer to hold capital rather than stocks, and supply chains are fragile.
With the shortest transport interruption, shortages in the rural network spread rapidly.
As official supply chains collapse, counterfeit life-saving drugs are beginning to take the place of legitimate ones; this introduces further dangers into already vulnerable systems.
A WAY TO STABILISE
Although conditions look grim, innovations offer some hope.
Through trials of long-range autonomous drone dispatch, pilot projects hope to break the bad news: that venom ferries are spreading throughout the country. At 1 km per hour across broken terrain in real time, emergency medicines and antivenom can now reach victims far more quickly. Early results indicate more dramatic cuts in response times than under present systems.
Also, citizens’ advocacy groups are standing up to lawmakers to introduce greater transparency into how emergency medical supplies are procured and distributed. Height gaps in public health are not only a matter of infrastructure; a level playing field must also belong to the people themselves.
Overflow. The core of this crisis is not a lack but a distribution. Treatments that save lives should not be a privilege enjoyed only by people living close to major roads or cities. An effective health system cannot make geographical location a factor in survival.
Until procurement reform, investment in infrastructure, and effective oversight are jointly in place, rural hospitals will find themselves fighting on empty.
Hostage to the last vial in his hand, a doctor is yet forced to make choices for the sick.
Introduction: “——–” I analyse a broader inequality between rural or township populations and city dwellers. This is one of our most urgent global issues.
This chapter turns its attention to problems with supply chain and procurement links, as well as to Taking Responsibility for Tomorrow, Schubert and others. Government, private industry and civil society together are all responsible for reform.
At The Bengali Roots, sustainable progress rarely starts on its own: we feel public discourse and full disclosure are the beginning. This survey will continue to seek views from legislators, medical professionals and the readers.